Opioid Abuse in Erie
Pain, grief, and resolve in the face of a rapidly escalating crisis
The numbers
The scale of the problem of opioid abuse in our country is genuinely alarming. Before I began working on this article, I knew about the issue mostly through its effect on people I care about. But I was deeply unaware of its horrible scope — and the degree to which it has escalated recently.
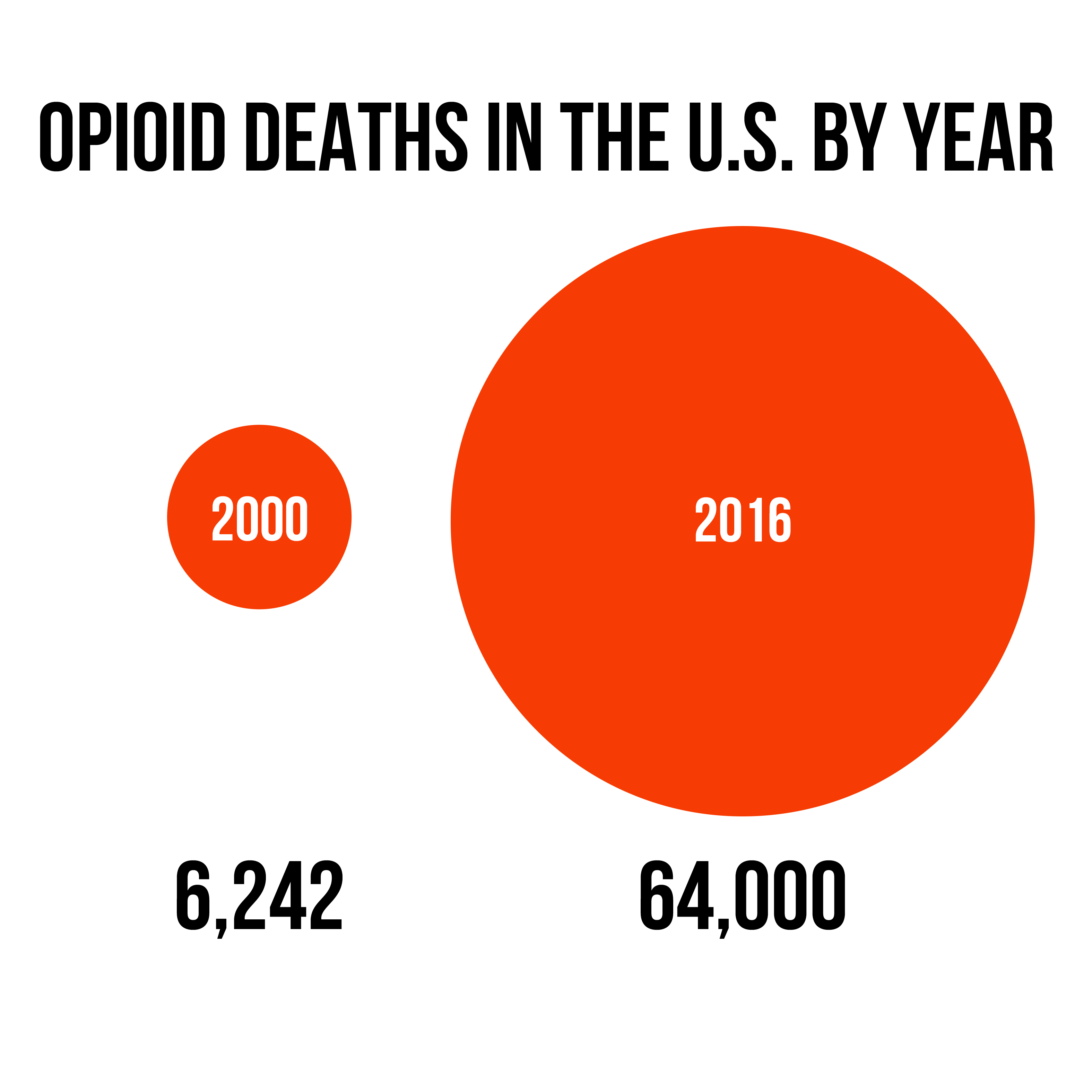
Let's begin with some astonishing numbers. In 2000, the Centers for Disease Control (CDC) estimated that there were 6,242 opioid deaths in the U.S. By 2016, that number had escalated to roughly 64,000 people — and that figure reflects a 22% rise over the previous year, according to the National Center for Health Statistics. Last June, the New York Times reported that "drug overdoses are now the leading cause of death among Americans under 50."
"Opioid" is a blanket term for substances that bind to the opioid receptors in our brains. Heroin is perhaps the most famous example, but prescription drugs like OxyContin, Percocet, and Vicodin are also opioids. And although the U.S. makes up roughly 5 percent of the world's population, the CDC estimates that we consume about 80 percent of the world's supply.
In Pennsylvania, the National Center for Health Statistics concluded that there were 3,797 drug overdose deaths between July of 2015 and July of 2016. In the year that followed, that number jumped to 5,443. The Pennsylvania State Coroner's Association estimates that "thirteen people die every day in Pennsylvania from drug-related causes."
Locally, the Coroner's Association tallied 95 drug-related deaths in Erie County in 2016. Opioid overdoses were responsible for 80 hospitalizations in our community (34 for heroin and 46 for pain medications). 2017 was even worse — there were 124 drug-related deaths in Erie County, according to our coroner Lyell P. Cook.

There's a lot of blame to go around for these numbers. A 2015 study produced by the Annual Review of Public Health concluded that between 1999 and 2011, "consumption of oxycodone [the active ingredient in OxyContin and Percocet] increased by nearly 500 percent." Between 1996 and 2002, Purdue Pharma launched a campaign to encourage the use of opioid pain relievers for "chronic non-cancer pain." Through sponsorships and grants, they orchestrated over 20,000 "pain-related educational programs."
Purdue also provided financial support to organizations like the American Pain Society and the American Academy of Pain Medicine — which in turn advocated for more aggressive pain treatment. There soon arose a plethora of physician-spokespersons advocating on behalf of opioid manufacturers, often using flawed evidence to argue that addiction rates were rare.
One especially notorious example of poor scholarship is the so-called "Porter and Jick" letter. In the 1980 edition of the New England Journal of Medicine, a five sentence letter-to-the-editor was written by Dr. Hershel Jick of Boston University and his research assistant Jane Porter. It noted that they had encountered only four cases of addiction while working with over 11,000 patients treated with narcotics. In response, a genuine desire to relieve people from chronic pain and a dangerously unethical profit motive became strange bedfellows, and the claim went viral. Despite being written informally at a time when narcotic painkillers were subject to rigorous controls, those five sentences were cited over 600 times in scholarly studies and journals.
Combine all of this with the growing sale of cheap black tar heroin from Mexico — often marketed to people who can no longer legally obtain prescription medications — and you have great cause for concern. Add the rise of illicitly produced fentanyl to the mix and you're talking about a major crisis. Fentanyl is a synthetic opioid that is typically 100 times more potent than morphine. It's often mixed into cocaine and heroin, and can be marketed as a counterfeit prescription drug as well. The CDC estimates that death rates from synthetic opioids rose by an astounding 77 percent across the country from 2014 to 2015. When I spoke to our coroner in early March, he noted that fentanyl played a role in the vast majority of drug deaths last year in Erie County.
If these figures are beginning to make you dizzy, I don't blame you. To scale down the problem, let's shift focus to one local person, his struggle with opioids, and its long-term effect on his family.
Skunk's Story
Steve Shaner was the kind of sweet, friendly guy that you might bump into at a music venue. Known as "Skunk" to his friends, he was a self-taught drummer who spent time in local bands like Triage Unit and Wandering Accident. He loved to head off to music festivals when he could, especially if Brothers Past, the Disco Biscuits, or American Babies were playing.
At Fairview High, he was in the marching band. After graduation, he enjoyed his work as a "bug man" for PDQ Pest Control. "He was someone you wanted to be friends with, and he truly had a huge network of friends, of all different types," according to his older sister Ann Fabrizio.
Steve also struggled with drugs for many years, which eventually lead him to heroin. "He was very secretive about his addiction. There weren't things I found at home that would lead me to believe he was using," says his mother, Deborah Shaner Little. Her suspicions escalated in 2014 after a close friend died of an overdose. Fabrizio recalls being "warned that we should be watching out for Steve," but ultimately trusted him when he claimed he wasn't using.
Later in 2014, as the addiction was beginning to take a toll on him, Steve decided to move to San Francisco. A close friend in the city offered to help him turn his life around — even offering to pay for the plane ticket to California. For a time, this decision paid off. "Steve got clean for a while and was very, very proud of himself for having done so," according to his mother.
Eventually San Francisco became too expensive and he left. After a few months in Florida with his father, he returned to Erie. By this point, he had resumed using. His mother feared the worst: "I was terribly afraid for him to come back here to Erie. I felt like it was going to be too much temptation to get back into old habits. He came back in July of 2016 and he was gone by February of 2017."
Corresponding with his family, I was struck by the enormity of what they had been through. The overdose that took his life was his third in five months. His mother found out about the first when a letter from the court system arrived in a mailbox they shared. When the second occurred, she found him passed out in their home and called an ambulance in time to save him. Less than three months later, she discovered him unconscious again in her bathroom. This time, he never regained consciousness.
"I want to bring attention to this because it is a critical part of the problem — he didn't feel like he needed help," says Fabrizio. "The opioid addiction he battled had truly affected his brain chemistry so much so that he was unable to see how deep in he was. We talked about meetings, he told me it was an easy way to meet new people who use. How disheartened I felt, thinking that something I thought was a viable option for help was so quickly struck down."
Although Steve wasn't able to find the help he needed, his family has been proactive in dealing with their grief. Fabrizio has two young children who struggle with the loss of their "Uncle Skunkie." Accordingly, her family and her mother have sought out counseling at the Highmark Caring Place, which offers services to young people and their families who are dealing with loss.

Steve "Skunk" Shaner, who worked in pest control and drummed with local bands, is one of the many lives claimed by opioid overdose at far too young an age.
Contributed Photo/Deborah Shaner Little
Steve's mother has also found support online, especially via Facebook groups: "Some of them are specifically geared toward loss from addiction. Some of them are for loss of a child. There's a lot of them out there." The Internet also introduced her to the Black Balloon Project. On March 6, Steve's loved ones hung black balloons outside their homes to make the issue visible, hopefully lessening the stigma surrounding opioid abuse.
In February, Shaner Little participated in an awareness campaign begun by a grieving mother in Brockton, Massachusetts to put a human face on the opioid crisis. On Facebook, 664 people pledged to send Valentine's Day cards to the president and our state governors. Shaner Little's handwritten letter to the president acknowledged her dismay that "her beautiful boy is one of the statistics of the opioid epidemic." As of this writing, she has received no response from any public official.
Providing Assistance
The Pennsylvania State Coroner's Association estimated that "there were 31.1 hospital admissions statewide for opioid overdose per 100,000 Pennsylvania residents" in 2016. In Erie County, that number went up to 35. Obviously, this puts a tremendous burden on our emergency rooms, whose care is often limited to short-term crisis situations. But a new partnership between our regional hospitals and our mental health facilities is creating opportunities to intervene effectively in these settings.
The Warm Handoff program began in October of 2016 as a way to connect people in overdose situations with mental health professionals as immediately as possible. "We have something that meets the person where they're at. And not just metaphorically where they're at with their substance abuse disorder, but literally, physically where they're at," says Mandy Fauble, Executive Director at Safe Harbor Behavioral Health.
Here's how the program works. Someone is admitted to a hospital for a drug-related emergency and receives medical treatment. Shortly after, case managers from Safe Harbor (working in partnership with UPMC Hamot) or Gaudenzia Erie, Inc. (working in partnership with Saint Vincent, Millcreek Community, and Corry Memorial Hospitals) arrive at the hospital to "connect them to the right resources," according to Fauble.
Fauble notes that once an overdose situation is resolved in the emergency room, patients no longer have immediate medical needs. "What they have is a need for substance abuse disorder treatment," says Fauble. "The goal is to refer them to the right level of care for them. That might mean drawing from any number of providers in the community. We might refer to the Center for Excellence or the Esper Treatment Center, for example." For Fauble, partnerships are crucial to the success of the program. "Providers really see themselves as part of a much larger safety net for people and there is a lot of collaboration among agencies."
The Warm Handoffs program is funded through state resources allocated by the county and requires no fees from anyone who receives service. When patients agree to seek treatment, the case managers provide guidance in response to a variety of everyday issues as well. This often means daily check-ins for counseling, assistance with housing transitions, and strategies for dealing with living partners who are also dealing with drug abuse.
As a licensed clinical social worker, Fauble is familiar with the obstacles that keep people from seeking treatment. She stresses the need to "recognize that substance abuse disorder is not about morality, it's about things in people's lives that put them at substantially higher risk." One example is the strong connection between drug abuse and personal trauma. "Eighty percent of women who enter treatment for substance abuse disorder have some type of trauma history, typically around physical or sexual abuse," according to Fauble.
When addictive behavior is rooted in medical prescriptions, this can also create barriers to recovery. "It can be hard to realize that the thing that helps you function can also hurt you." Fauble stresses that relapses should be handled with empathy, because "it often takes more than one time for people to be in recovery." Above all, she thinks it's important to avoid isolating and judging people, especially since "25 percent of Americans at some time in their life are going to deal with a mental health concern."
Raising Awareness
The Jefferson Educational Society recently made the opioid crisis a major priority in its mission for "community progress." According to Executive Assistant to the Director Angela Beaumont, "it had become clear that the national opioid epidemic had started to show an obvious local presence," which encouraged them to take action. Accordingly, the Jefferson's 2017 Civic Leadership Program, which encourages young professionals to examine "Erie's economic, entrepreneurial, and innovation ecosystems," was devoted to raising awareness about the issue.
The Jefferson Educational Society's 2017 Civic Leadership program dedicated itself to examining "Erie's economic, entrepreneurial, and innovation ecosystems" — curtailing opioid abuse and helping those afflicted was identified as a key initiative. The #ErieOpioidProject encouraged those affected to step forward and share their stories.
The 23 participants in the program identified "stigma" as a key area of focus. "We wanted to reduce the stigma of addiction," according to Natalia Garcia, a producer and director at WQLN. "We thought that if it were easier for an addict, or the family of an addict, to talk about what they are going through, they would be more likely to seek help."
The participants split up into four teams, focusing on production, administration, reporting, and research. "As a group, we decided the best way to 'break the stigma' surrounding addiction was by telling stories through video," according to participant Jessica Yochim, owner of the local media company MenajErie Studios. "We interviewed former addicts, parents of addicts, and healthcare professionals."
Tyler Titus, a licensed professional counselor, stresses the importance of clear parameters for the interviews. They avoided speaking to children and people currently struggling with addiction, out of fear that the content might trigger a relapse. "We wanted to show people from different walks of life and different backgrounds and different recovery journeys. We wanted to highlight the various struggles while not losing sight of possibility and hope," according to Titus.
Their work, which was ultimately shared across social media through the hashtag #ErieOpioidProject, eventually took the form of 12 video interviews which can be viewed on the Jefferson's website (as well as on YouTube). Working in partnership with WQLN, they "interviewed former addicts, parents of addicts, and healthcare professionals," according to Yochim. According to Natalia Garcia, their team didn't "want to control the narrative of this project. We let the participants talk as much or as little as they felt comfortable with." In response, the interviewees were remarkably forthcoming — detailing struggles with homelessness and the loss of children, for example. There are also firsthand accounts from professionals dealing with the issue, ranging from think-tank researchers to pharmacists working to ensure that prescriptions are administered ethically.
When asked about what she'd learned from the #ErieOpioidProject, Yochim notes that "there are a lot of resources locally that are available to addicts and those affected by addiction. I think the best thing we can do is keep the conversation going and offer support by whatever means we can." To move forward as a community, Tyler Titus thinks that "we need to address barriers to services. We have segregated communities and we need to acknowledge this and be proactive about it. We have poverty pockets that face systemic discrimination and this further compounds the issue of stigma and addiction."
I can't conclude this article on a positive note. Frankly, I suspect that opioid abuse is going to get much worse before it gets better. But there are plenty of local people working very hard to raise awareness and to connect people to the resources they need. In fact, there are dozens of local initiatives I had to edit out to complete this article. Better still, our community seems largely dedicated to addressing the problem as a public health crisis rather than something we can brush aside through mass incarceration.
When I asked Ann Fabrizio, Steve "Skunk" Shaner's older sister, what she felt was necessary to fight opioid abuse in our community, she was very forthcoming: "I want our government to realize the severity of this problem and to start initiatives towards helping those struggling. I want to see more treatment options available for people who may not have insurance.
These strike me as good suggestions from exactly the sort of person we should be listening to.
Dan Schank can be reached at dschank@eriereader.com